|
7th April 2020:
Today was the first day of the "emergency" rota in our dept. It was hauntingly quiet, like coming in on a Sunday given that our outpatient department is only open Monday to Friday. 2 doctors (one was me), 3 nurses doing leg ulcer dressings, and 3 secretaries. It was the most opportune moment and productive day that I have had in weeks/years to sit down all day behind a closed door with just my computer for company, and catch up with my admin. After the hands on busy long days leading up to this, all my follow up patients have been cancelled, including skin cancer patients, I have had a pile of results to look through and patients to contact with these, and I need to plan for my patients who have been put on hold. I also have to familiarise myself with our whole skin cancer database in my new role which I have taken over from our cancer nurse specialist for the time being. Two of my consultant team came down after their morning on the ward-they still had marks on their faces from the masks. They said it was ok, that the respiratory consultant discharged two patients, that they were learning a lot, but that while the wards are still well stocked with the medical teams both senior and junior, they were a little surplus to requirements, so came down to catch up on other work like I was. Worryingly they said that many patients aren't adhering to the advice of covering thier mouths when coughing, and wearing their masks as neck or mouth warmers, which is entirely inadequate. There is just so little control of what are essential details, which could change the face of this crisis so easily, one way or the other. I cycled home and freed myself of the day's thoughts, home to my caring husband, and threw myself into cooking home made burgers of epic proportions-cooking (and eating..) new recipes have become my relaxation it seems. As is watching daily episodes of Modern Family-escapism with humour, it's the antidote to these times of otherwise pensive contemplation. Glad to also hear that Boris remains unintubated and breathing consiciously. St Thomas' hospital will be deservedly praised for their supreme care of our Premier, as should all our hospitals continue to be.
0 Comments
6th April 2020:
I spoke to our skin cancer nurse specialist today as I've been nominated to manage the skin cancer database for our department as she has been drafted to work in itu this week. Some 20 years she hasn't worked up there she told me. But the mere fact that she has the experience is what is taking her up there now to be one of our heroes. My equally heroic team started their rota on the palliative covid ward today. If only a hand could be held up there, where relatives aren't even allowed to see their dying loved ones. I know my team will do some (gloved) hand holding, and covid and the rest of their ppe won't work as any more of a barrier to give someone dying the compassion and comfort they deserve. I wish I could be up there with them too. The other side of things on the ward they are working on is that it also houses patients who are relatively well and after some assistance with oxygen therapy will be going home. Discharging patients home is an upside to a ward round on any given day, and in this current clime the best it gets. 2 days ago my hospital closed its doors for 12 hours due to their depleted oxygen supplies. Yesterday the queen addressed the nation in a rare impromptu tv speech. Today our PM got admitted to hospital as he was still unwell with covid symptoms around a week after contracting the infection. Tonight he has been escalated to ITU. I hope when I wake up in the morning he isn't on a ventilator. Sent from my iPhone Monday 4th April 2020:
My GP friend has been doing home visits in amongst her remote consultations with patients. They were all palliative covid patients. It seemed so wrong she said. I read another moving piece: "And People Stayed Home: And people stayed home and read books and listened and rested and exercised and made art and played and learned new ways of being and stopped and listened deeper someone meditated someone prayed someone danced someone met their shadow and people began to think differently and people healed and in the absence of people who lived in ignorant ways, dangerous, meaningless and heartless, even the earth began to heal and when the danger ended and people found each other grieved for the dead people and they made new choices and dreamed of new visions and created new ways of life and healed the earth completely just as they were healed themselves." The poem's author Kathleen O'Meara wrote this after the famine in 1869. And never was it so true of our year 2020. Saturday 3rd April 2020:
I'm loving the opportunity to have some time at home with my husband, and enjoy our permitted hour in the great outdoors. He has been running or cycling each day, and today I cycle alongside the 10 miles that he is running! To feel the air in my lungs reminds me of how lucky we are to be here, to be well, to be exercising, to be alive. It has been hard being at arms length from him-whilst I've been working I've been so cautious not to kiss him! I have moved him to another bathroom in the house, and I keep doing all I can to prevent entry of the virus to our home space-I take my work clothes off at the front door, they go into the washing machine at 60 degrees, and I go straight to the shower and wash my hair every day that I've been at work. And I've been doing this before the respiratory consultant told us that she has been doing the same. It seems a new revelation to many of my colleagues. I really haven't been taking risks! We come home to messages that my hospital has declared a critical incident and closed a&e to all patients. It makes the national news. My hunch is that it is as the resp consultant said to us on Thursday-that oxygen supply was running low. Who knew they could. But in a crisis caused by a virus which overwhlems the respiratory system, and in the numbers that it is affecting, and the time it takes to progress with these patients, this isn't actually surprising. It turns out that this was indeed the case, but they managed to replenish safe supplies and reopen the a&e by that night. All patients in the hospital had safe amounts of oxygen available to them, but to remain that way the had to divert any new demand on it. Unprecedented-never have I heard or used this word so many times. But the decisions being made in our hospitals all over the world are at a level most of us may not be able to imagine. The Nightingale Hospital officially opens at London't Excel Centre. 4000 beds for covid patients has been built in just 9 days, a phenomenal effort with the help of some 200 soldiers. Who knew that this could be done. I had doubted anything like this could happen when I saw how they did the same in China. A great use of an empty shell of a building, but I look at the scale, and the equipment, and the strained staffing levels in our busy hospitals, and wonder if and how much it will be used. I hope that the good planning is only in anticipation, and that this vast hospital doesn't come into use. And if it doesn' then what of all the equipment getting dusty? Hopefully it will get to where it is most needed, even if it doesn't turn out to be the Nightingale. Still an overwhelming effort. Thursday 2nd April 2020 :
Today I brought a roll of cling film to work-I played with the idea that I could fashion it a long sleeves and wrap it around my arms, and dispose of it between patients, as a substitute for lacking long sleeved gowns to operate in. It becomes fiddly, embarrassing, and I think may carry risk of shedding any virus when doffing (removing). I return to scrubbing up to my upper arms where my short sleeved scrubs sleeve stops. And now we are also taking our scrubs home to wash as there are none left in the department.. We have the first proper and beyond brilliant session with a respiratory consultant who came to the dept to talk to our team. I was in awe at her calmness and coolness. She explained more in an hour of what is going on with covid in our hospital than anything we have known all these weeks. In one hour she managed to reassure and also take the pressure off my lead consultant who has been a swan calmly gliding across the surface whilst kicking her feet frantically under the water. But you would never know. And that’s what makes a good leader. But today the team spirit was incredible, the pulling together, and the support in that one room, not only amongst us but also with this expert in the frontline specialty helping run what is a seamlessly oiled ship looking after covid patients in our hospital. How could she stay so cool and calm and sleep through all this I asked. She laughed . And said covid is an easy disease to manage as it is so protocol driven. Even though the sad reality of that is the decisions are based on those patients who will live and who will die . And we have already heard of staff members dying in our hospital. Even though I'm now not being deployed to the wards, the feeling of reassurance amongst my team after this talk was palpable, to know that they will be supported up there, that they will be in relatively low risk environment, and that they won't have to make major clinical decisions, was like seeing a pressure cooker releasing its steam. Some of my team walked down the corridor and stepped out of their offices to follow the laughter that was coming from my room. "It's great to hear laughter in the department right now, something we aren't hearing enough!" one of my consultant colleagues said. As we shared jokes and videos, it was a moment I held, and if I couldn't physically be on the wards with my team, I would work my hardest to keep our skin cancer patients on the radar, and keep some humour going at the very least! I'm moved by a pieces I have read, sent from a friend: We fell asleep in one world, and woke up in another. Suddenly Disney is out of magic, Paris is no longer romantic, New York doesn't stand up anymore, the Chinese wall is no longer a fortress, and Mecca is empty. Hugs & kisses suddenly become weapons, and not visiting parents & friends becomes an act of love. Suddenly you realise that power, beauty & money are worthless, and can't get you the oxygen you're fighting for. The world continues its life and it is beautiful. It only puts humans in cages. I think it's sending us a message: "You are not necessary. The air, earth, water and sky without you are fine. When you come back, remember that you are my guests. Not my masters." Thursday March 26th 2020:
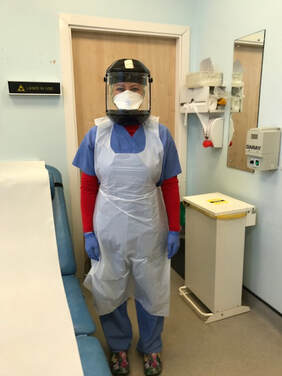
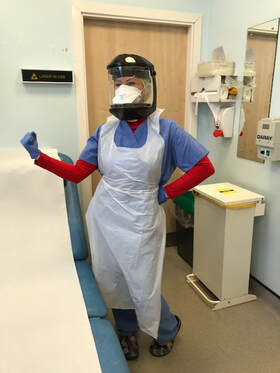
I slept badly last night. It is another busy day operating at work, but I know I'm not experiencing a fraction of what the other teams looking after the covid patients are. They are suffering. I know from a nurse friend who used to work in our own hospital ITU and still keeps in contact with her former collegues up there, that they are getting pressure sores from wearing the protective masks for so many hours a day caring continuously for the sickest covid patients during their 12 + hour shifts. I feel like a total shrimp doing what I'm doing compared to what they are all doing, I have no doubt that the amount of support they are giving each other up there will be better than most teams anywhere as they wade through their daily grind. I also hope that they are getting support outside of ITU, time out to rest, to reflect, to offload, to find joy with their families at home,. Lockdown in the UK has been taken on, schools are closed, with children are being home schooled, and people are working from home. Many things are on tv advising on how to make lockdown a pleasurable/educational/ nourishing/healthy/fun experience. I've not been home much as I've been working through my leave which had been booked some time ago, but it doesn't seem right to be at home, and with many of our team in the department self-isolating (themselves or family members with one or more covid symptoms, the lack of testing means they are forced to be at home under the current advice. I admit I am finding it hard to hear of people enjoying their lockdown as though it's a holiday, a staycation. I don't begrudge them, of course I don't, we need to keep this country upbeat and continuing to thrive beyond the depressing news everyday! And Boris and his team are doing a great job of the live daily updates in a way that keeps the nation informed and opening themselves to the questions that so many are asking (although noone is uttering the word Brexit anymore!). I ponder that ignorance is in fact bliss . I wish I was ignorant to it all. Inside knowledge and close proximity to the realisty is what creates the stress. It doesn't feel like it should be a time to party. And that's my issue to deal with in my own head. Dad shares a covid reporting app today which I promptly share with all my friends . I then find out it is my colleague’s husband who set it up. I make sure we and my family stick to a rigid daily report on it . Genius idea. As is much of the work this man does. And he’s on bbc news talking about it. It was decided at our team meeting today that I won’t be deployed to the wards for certain. Much to the relief of my husband and family. Much to the lack of honour for my comrades to be deployed while I stay working in the dermatology department. I know it is not something which will easily be overruled, and I also know that some of us need to stay back to keep the derm dept running, and we will be spread out in what, where, and how we do this. Things for us are changing daily. My lead consultant is doing such an amazing job under huge pressure, to answer so many questions from the hospital leads, and the staff she oversees, and doing this whilst juggling the clinical work too, has been a feat of some size, but she has managed it calmly and elegantly. We are all behind her. We will do whatever it takes in each of our roles to make this whole thing as seamless as possible. Working in different ways, whether on the wards or in the derm dept or elsewhere is going to be our new normal for a while. Tonight is the first clap for nhs - it’s overwhelming . So many people out and videos from friends sent to us too. I see the emotion in my husband's eyes as he claps furiously on the balcony of our flat along with many others on our development. I can’t stop my tears. They are the heroes on the frontline. Not me. But I feel nothing but utter pride for the institution that I work in, and long may it survive. I hope that this time makes us and the whole country take a long hard look at the way it has been running for so long, and with so much dedication and goodwill. We are seeing that A&E departments can be empty of minor things, ambulances can be left to do only the emergency work that they are meant to do, GP’s can see only the patients that they absolutely need to, dermatology departments can also do the same, and IT departments and hospital trusts the nation over can enable digital systems at the drop of a request without a hundred meetings telling clinicians why they can’t have permission to use a digital system for remote and more efficient triaging. The NHS can change after this, and for the better good of the people who work in it for the people who need it. I pray for greater change in this institution so we can keep it going, but that will require changes in people’s mentality at all levels of the profession and also in the public. The NHS was broken, morale was low, but work ethic remained high. And here it is again for all to see that despite its suffering it defies any other organisation in its ability to fight and to work and to provide for its most needy. Please let us rebuild it in ways that make it indestructable in the future. Wed 25th March 2020: I decide to get armed and repel the danger of coronavirus in my own way at work-there just doesn't seem to be the same sense of urgency in our department, and it hasn't helped that the measures we adopted (to take patient temperatures, clinic staff to wear basic protection in the way of scrubs, aprons, and simple surgical masks) are being refuted by a senior hospital matron. I find this unaccepatable that our nursing staff have been told not to wear any protection "for fear of frightening patients". I overrule what I am hearing from our precious nurses and tell them to continue and I will answer to whoever is suggesting otherwise. On the contrary, all my patients who have been attending for their surgery, (some in their own face masks, others we give one to), have expressed only gratitude that we are still running our service for their more urgent need. And they have said how reassured they have been by our visible measures to confer protection of them and of ourselves. These people fear this virus, not of seeing the donning of physical protection amongst staff which is what they have seen everywhere else on the news. Physical examination and treatment of patients requires close proximity between clinicians (doctors, nurses, healthcare assistants) and patients. Spacial distancing is impossible. If I were a patient I would be acutely aware of how many people a clinician treating me would be coming across in a day, and I would want to have a decent barrier between us. Some patients haven't attended their clinic appointments because of their concerns with exposure. I can't really blame them. I take things up a notch from my paper surgical facemask, and borrow a visor usually used for UV phototherapy by our nurses (it makes me wonder even more why anyone would ever consider lying on an artificial sunbed when this visor is used to protect the nurses during controlled uv treatment of patients). I feel the safest today than ever before, but the FFP3 mask (of which we have only a few) is marking my face after wearing it for an hour, and with the visor on top (which makes me sound and feel like Darth Vader in a sauna) makes for a heavy day’s operating. But it raises some smiles, even if people think I’m overreacting in my little dermatology dept. Granted we aren’t itu. And my thoughts are very much with my colleagues up there. But there’s no risk worth taking right now I feel. Even in our dermatology department, and especially during facial surgery. I wore a long sleeved high necked top under muy scrubs today as we don't have long sleeved gowns, and I feel even more guilty asking for these when others in the hospital need them. I keep a separate pen for my patients to sign their consent form, and I sanitise it afterwards. The door handles are wiped down with each entry and exit into the op room. I don't think I'm overreacting. Am I?? I go home tired today. And emotional for the first time. The impact of what’s going on is hitting me hard this week. I can’t help thinking about what is going on on the wards and itu and in A&E and in places we aren't hearing as much about like care homes. I think about the fact that the dying and their relatives are not together, and that funerals can't even be attended in the usual way. I think about the fact that patients with cancer are amongst the people who are being delayed or even denied their treatment. I cry when I get home as I think about the seriousness of this pandemic now, having been so calm and pragmatic and reassuring my colleagues as much as possible, when all along I’ve been slowly gaining a momentum of a background anxiety myself, and tonight it bubbled over. I wept on my own.
My husband wanted to comfort me. I said that I was finding it hard to verbalise what I was feeling right now, but confused, worried, sad, anxious, helpless in a situation out of our control, uncertain, guilty, and not believing what these covid patients, their worried families all at a distance, and cancer patients and other sick patients must be feeling. I think of the devastation my family and I would have felt if I was told when i had my cancer diagnosis that I couldn’t get my treatment at that time, and how lucky I was to have access to such treatment. I then think of those who can’t afford it, can’t reach it, their illness too advanced to be given it, living in places which don’t have the science, technology or funding for it, whether here or in any other developed or underdeveloped country. And then I think that horrifyingly this must also be true for covid-19 right now. And across the world. It's 4 weeks to the day since Ash Wednesday, when I gave up chocolate, cake, and sweet things for Lent. It was a chocolate day today. My husband and my friend, who both know me too well, give me permission to break my resolution early.. so I do. My night is complete. Tues 24th March 2020:
Today I took the decision to close my private skin surgery service and which I do from a local private clinic. The only other time I have paused this since I set it up in 2010, was when I went to Canada in 2017 and after 9 months I came back to a busy time where loyal patients had wanted to wait for my return. In the interests of patient safety and in line with government and Public Health England's advice, I didn't want to wait any longer to decide over this. None of the surgery I do in this service is urgent-my role is rather more that of Dr Pimplepopper, as I am locally becoming known as! I have to lend me energies to the urgent skin cancer in my NHS job, and await news of deployment. All my booked patients are understanding and seeminly relieved at the decision, and I hope to pick things back up when it is safe to do so again. While I’ve been operating full skin cancer removal lists at work and so up close to patients I have been remaining always aware of my unknown personal risks after cancer in my chest which required chemo and radiotherapy as well as a stem cell transplant, I have had to self risk assess and have again remained ahead of the advice curve and have been trying to champion the need for Personal Protective Equipment (PPE) for all of us in dermatology. And all the while being so aware that it is in short supply so why would anyone in dermatology be considered above anyone in itu? It’s a sad reality, but putting some doctors and their contact risk above other doctors is why doctors, and nurses, are dying. It may be easier to consider that known covid patients being admitted or treated, or sadly dying, are the ones to protect from. But what about those without symptoms who are shedding it every time they walk into our outpatient dept, our operating room, every time droplets from patients coughing, or from the aerosol generating particles (AGP) produced every time we cauterise bleeding vessels during our surgery, enter my operating room environment (and in dermatology these rooms are smaller and the ventilation requirements are less compared to proper operating theatres) I still think we are as at much risk as anyone. My husband and family have been urging me for weeks not to work directly with covid patients, concerned that I may be more vulnerable after my lungs and chest were the focus of my previous cancer and treatment. My manager had submitted a referral to occupational health as she and my team appear to have the same concerns. I was a bit timid to even express my husband's concerns to my manager about my previous illness, and I'm a bit resistant, almost embarrassed, to be presenting myself as a risky worker, when all I want to do is help however I may be needed. I don't want to be seen as the one who didn't put herself forward, the one who couldn't didn't help her comraces. I feel well, I’m careful with my protection, and have been for longer and more seriously, than several of my dermatology colleagues, as I assumed a slightly higher risk to myself, and I’m definitely doing procedures which bring a bit more risk to my working day, and we don’t have all the right gear. Yes I’ve been fit mask tested and will now get on with using the new mask, but I need to think about a visor, long sleeves, donning and doffing (putting on and taking off ppe) carefully. As a department we have started taking patients' temperatures on arrival, the staff wearing a plastic apron, gloves and a surgical mask during the daily grind, and I've just made sure of taking all the precautions I can in the op room for myself and my assisting nurse. Noone is really telling us to do this in dermatology outpatients, but why wouldn't we? We still need to take individual responsibility to protect ourselves and our patients-we still can't see with our eyes where this assailant is, so why wait to be told? I attended a webinar tonight on covid by an itu consultant in Edinburgh with my friend and surgical colleague-more for my own education on it, and not because I think I’m going to managing these patients, given the hovering suggestion that I may not be selected to go on the front line. I am so privileged in my job to treat the generations above me, who have taught me so much, and could teach all our generations so much more, including in this health war. So many elderly male patients of mine who have talked about their time fighting in a world war, have been nothing short of heroic, in whatever roles they had to adopt, whether serving frontline in the trenches, in the air, on the sea, or unseen working with intelligence and in the planning and administrative roles behind the visible scenes, at all levels of rank. I always comment, with deep gratitude, on their blazer pins which many still so proudly adorn on themselves, as this small symbolic reminder to themselves and to those who recognise the significance of this 5p piece sized badge, is the one reminder of what they did to bring us to the place we all have the privilege to be in now. However many others have told me how they couldn’t join the army/airforce/navy due to a health condition (we specifically ask if they served when we are treating their skin cancers, as a war veterans agency exists which compensates former servicemen for their time served in hot countries in the war and if they have subsequently suffered a skin cancer. It is the least I can do to inform them of a potential opportunity for a monetary bonus for what they did for us). I have learnt that those who weren’t allowed to sign up, without exception, still feel guilt and disappointment even in their 8th and 9th decades, and so many years after the war ended. And now I have an inkling of what they felt like to not have the opportunity to serve at the country’s greatest time of need. But better to live a coward than die a hero as they say. Maybe so for some, but not for all. This would never have been said to me when I had cancer. When facing mortality then had a different meaning, because I wasn't volunteering myself to get cancer, I was only working hard, with all the help I could get, to fight the assailant. Would I be a coward, or would I be sensible if I were not to step forward, or not be stepped forward, to help in this war fight against covid? I still can't consider not being in it, and still intend to play my part, whatever role I am summoned to have. I reflect again on our war veterans. Many talk with such pride and commeraderie, whilst others remain silent and have lived with post-traumatic stress ever since. Everyone's experience of the same event have been so different. I imagine the same with this millenial world event. I learn a lot from the webinar. I don’t like that people are getting hypoxic after 5 days and by staying at home at the moment many are presenting to hospital late and in a more serious condition. I fear again for my family. I’m 2 hours away. My dad is on the high risk list given that he is 76 with hypertension and copd. I pray he nor my mum come within a sniff of this virus. I order a pulse oximeter during the webinar and send it to my parents -this way they can measure their oxygen levels at home with a finger probe and know if there’s a problem quickly and not to wait to get to hospital. I pray hard again that none of this advice I’m giving them ever needs to be employed. I also write a message to my younger brother, a hero to me, perhaps because his distance is more painful for all of us than for him right now, and our ability to reach him is so limited. I try to encourage him to keep in touch, I tell him that we may need him and he may need us. I ask him that now we all segregated by force, and with no knowledge of where I’ll be posted in the coming days to weeks, I hoped he would keep himself safe, and be reassured and be reassuring to us, that he is ok, that we are ok. I know my brother, although in the film industry, doesn't watch much TV, and this is where we are all getting the covid info as it emerges. I don't expect a reply, and I don't get one. Not to that message anyway. But again I just have to hope he has heard me. I am also worried about him looking after himself well through all this, and the knowledge that I can't have the same level of interaction with him as I have with the rest of my family, is hard, but it won't stop me letting him know what's important as things emerge. He is so precious to all of us. Monday 23rd March 2020:
Prime Minister Boris Johnson declares the uk in lockdown. I couldn't see this To me, this now means war. Yet I feel that we are being kept in the dark at my hospital-surely we should as staff be informed of the developing situation regarding our capacity for covid patients, our itu beds, how soon we will need to change what we are doing , or help out outside of our own departments (aka outside of our comfort zones)? With everything escalating in the media, it feels entirely hidden from us at my hospital, and with scenes are we seeing, it can't just be happening everyhwhere else and not where I work! Why the silence? I wake up feeling anxious, not only for myself but for all my colleagues, doctors and nurses alike. I feel compelled to write to our medical director to enquire about what the situation is with us. I have a pang of guilt as his job is immense at the moment, and whilst we are regularly being updated on covid protocols, advice, including that from the government, personal protective equipment, etc on our Trust internet, we have had no word of the actual or impending situation where we are, and that is becoming intolerable unnerving. Will a button just be pressed and everyone runs into action? How will they tell us when and how we are needed? It feels wrong, and we feel uninformed. The anxiety levels in myself and my immediate colleagues is rising, particularly over the past week, and amongst our nurses is as sky high as their morale is rock bottom with the lack of information, and their own fears of working on the wards-many of them left shift work on the wards to work in outpatients years ago, and this potential threat to their status quo is now raising enough of their concerns to resign if they are moved. As a doctor I feel we need to keep our nurses informed, and support and encourage and protect them, but right now we have nothing to tell them, and that feels disabling. We don’t know how to manage patients with covid, we don’t want to take the virus home to our loved ones, we fear the changes it will bring to our familiar hectic working lives in ways that we all fear. And never did we think we would be facing a health war of this scale in our entire careers. We don’t have a means to be tested yet, and I’m convinced the lack of testing has led to too many medics continuing to work on the frontline in Italy and scores of them sacrificing their lives to care for the patients whose lives they are trying to save from the same disease that they too have ended up being buried with. Excruciatingly families can’t visit their dying relatives due to the risk of the virus upon them, and so many people are dying and grieving alone. This is heartbreaking. With my manager’s support, I find my (written voice) and send the email to the man at the top: Dear Medical Director, As a non-consultant doctor in dermatology, I would like to share my concerns with you, having shared them with my manager, about the current lack of information being conveyed to the clinical work force as to the existing situation at this hospital regarding numbers of covid cases/itu capcity etc, and whether things are escalating behind closed doors without updated information being given to the very people who are required to assist if things are becoming overwhelming without our knowledge. I’m sure I speak for many when I express that I feel strongly that the trust have a duty to tell their soldiers the situation, which we have good reason to assume to be mounting, as at the moment everyone currently outside of the acute care situation is a sitting duck, and would appreciate clarity without wondering and thinking if or when we are reaching a tipping point here, and will be deployed outside of our specialities to manage these acute patients. Whilst there may be a feeling at the top that keeping us informed may incite panic in the workforce, this is in my opinion very short sighted to think that panic will be the overwhelming response if we are told where we are in numbers today, and every day. On the contrary-what we need to do right now is prepare, as individuals, as teams, and with time, however short now, to learn and educate ourselves if there is some undoubted certainty that we will all be called into battle. If the emergency button is suddenly pressed, and we are called up at the final hour and without training or preparation, then this will be disastrous for patients and clinicians alike. And that is when you will see panic... None of us have been tested, and whilst this is a vital intervention, without which we can all freely and hugely impact on our own and therefore our patients’ safety, I realise this is another battle we can’t overcome immediately as testing is not freely available. But I urge you-being kept in the dark is absolutely wrong in my opinion, and with the inside knowledge that things aren’t rosy in our locality, makes me even more sure of this, and if others were more aware of the current situation I’ve no doubt they would feel the same. These may be the thoughts of a mere clinician at the bottom of the hospital food chain, but who still has a soldier mentality of wanting to do whatever it takes to enable a favourable outcome through this war. Of course we all appreciate your invaluable ongoing considerations of everyone involved, and we know that you are also overwhelmed with all that is going on, it must be an impossible time for you. But I ask you please not to minimise our professionalism and overriding duty of care which we are all continuing without question to embody, now as always, but see this as a personal plea on behalf of us all, for information to be given to your army who you will need to be prepared, and who are likely panicking more at the lack of information of the current situation. Thank you, and I hope we can all have more transparency, as we work to prepare for the worst. Yours sincerely, Miss Sam Anthony Although I also feel like signing it off as "little old me, in cushy old dermatology, and anyway who am I to reach out to the medical director when I have such a meek place in this profession, and with greatest of apologies for bothering you at this terrible time". However my thoughts on the matter get me over that, and I feel he is the only person who could respond to this. And I press send. What's the worst that can happen I ask myself. It's unlikely I will be sacked. I may get thought of as an anxious worry-wort, someone stepping out of line and thinking I can weigh in with a moan to the upper eschilons of the hospital at a time when I should be quiet and get on with it, my colleagues may consider me to be interfering at a level not at all appropriate, I mean, I'm not even a Consultant, so what right do I have to tap in where Consultants have more authority to. All questions I asked myself, but what really in the end did I have to lose even if all this did turn out to happen? Well I wasn't thinking of myself in this, I was thinking of my colleagues. The dear man takes a moment to acknowledge my email and replies: Hi Samantha, We are launching extensive comms today, in this very fast moving situation. Apologise I can't give you a lengthy reply, but I'm really really busy. Apologies that you feel out of the loop. Best wishes, I thank him greatly for his reply at what must be again an impossible time. All I can do is speak out for the workforce as I have seen and felt for myself first hand what people away from the frontline are feeling, and wondering if/when they will be called up to serve in this war. Sunday 22nd March 2020:
It's Mother's Day. Perhaps against my own advice to keep far away from my parents for fear of unknowingly transporting any semblance of the covid virus to them, I have a feeling that if I don't take this opportunity to see them now, even breifly, and from a safe distance, if it really comes to our country locking down then it will be who knows when that I can see them. They live over 100 miles away, so for us it has never been a case of popping by for a quick hello ro a quick meal, it takes a bit of thought to make the nearly 4 hour round trip. That has never stopped me making spur-of-the-moment trips to my family home, even if only for a few hours, as to me, and it wasn't stopping me today, but it was the responsibility of ensuring that I don't inflict unseen harm in fulfilling what was my need more theirs at this concerning time. They were happy to stick with Facetime, but for me, seeing my family is hugely important for me, and the only way I can really assess how ok they are! And if anything I had a strong instinct to take them the hydroxychloroquine. We pass by my Aunty to drop off some things including the emergency supply of the drug too. My small way of saying I can try, with whatever I have and know, to protect them all. I also want to do the same trip to Stoke-on-Trent next week to my in-laws. We get to Bournemouth and Mum appears from the back door, and I deposit bags of things for each other on the driveway and don’t go within 2 metres of each other, while Dad stands chatting to us at the front door. It's rather comedic. We decide to walk down the side of the house to sit in the garden together, and mum brings lunch out . We all sit scattered around the garden which I’m grateful my parents have, for their sanity during this recommended isolation time, as much as enabling today. My parents have self isolated and socially distanced from each other for years, so I’m not worried that this period will do any added harm! I don’t step foot inside my parents house, and only wee once I get back home, impressive for an 8 hour round trip lunch included. It was a dry and sunny although cool day, and we chat and catch up, and laugh whilst we tyr to manoeuvre around each other and take it in turns to get our lunch from the table outside! It's like we are in some comedy sketch and not of this time. Around 4 hours later, we wave off through the window and front door. I’m so pleased we did this, it made the world of difference to us all. But I come home worrying I’ve left some virus from me from work in Bournemouth, and I start to fret. Rich reminds me that we kept more than a distance all day, and reminds me that I didn't pee all day becuase of it, and my paranoia did make us all laugh today. We watch the news and are appalled to see how brits everywhere crowded beaches and parks today with very little thought for social distancing. Because it was a sunny day. And it happened to be Mother’s Day. Yet still not seeming to understand the impact on the spreading of the virus from their actions, and when delaying the spread is all that we are being asked to do. Yes I feel that I went out of my way to travel to see my family, but not once was I not considering the distancing. I watch this and simply see a population going into a warzone with invisible bullets flying all around them but without any battle armour or weaponry, and I feel horribly sure that so many are going to succumb without a reasonable doubt. If only they could all see this invisible enemy. This is a national disaster. Surely the government has no choice but to lock down the nation now. Beacuse without rules, it doesn't seem to be phasing a large number of people here despite seeing the horrors elsewhere in the world. I go to bed fearful of what is to come. |
By Dr Sam AnthonySurvivor of a career in medicine, a career break from medicine, cancer, and blogging..join me in my quest to make us happier healthier individuals and doctors |
 RSS Feed
RSS Feed